SERVICESFOR HER

The basics
Options
Advanced options
Fertility preservation
Female Fertility Surgery
Female Fertility Surgery is the only type of fertility treatment that provides dual benefits both to your fertility status and to your general health as well. It addressees the underlying cause of infertility and targets it directly, offering immediate improvement. Female Fertility Surgery encompasses a variety of different operations, surgical techniques and equipment.
Fertility surgery is recommended in cases where a gynaecological or other condition affects the anatomy and/or function of the reproductive system, resulting in female factor infertility.
Gynaecological conditions associated with Infertility
Uterine fibroids or leiomyomas are benign tumors located in the myometrium, the muscular wall of the uterus. They are very common, occurring in up to 8 out of 10 women, they are frequently multiple and tend to grow in size and number as time passes, particularly during a woman’s reproductive years. The clinical symptoms that they cause depend on their number, size and location within the myometrium.
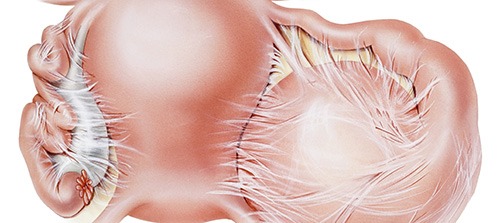
In the context of fertility, leiomyomas located close to the endometrium, the internal lining of the uterus, have been shown to negatively affect embryo implantation. Additionally, large uterine fibroids may lead to restrictions in the size of the uterine cavity, thus affecting embryonic development and they may also impair uterine constriction function, thus possibly leading to maternal.
Endometriosis is a common benign disorder that affects approximately 10% of women in general and up to 30-50% of women with infertility in particular. It involves the development of endometrium-like tissue (tissue that resembles the internal lining of the uterus) in areas beyond the uterine cavity. Such areas are frequently the exterior surface of the uterus and its surrounding ligaments, the ovaries (where endometriosis is called “endometrioma”), the intestinal tract and urinary bladder.

Endometriosis foci grow following a cyclical pattern based on the menstrual cycle and cause inflammation and fibrosis on the surrounding tissue. In the context of fertility, this is most destructive in the case of ovarian endometrioma, which impairs ovarian function, although research has shown that even endometriosis outside the ovary impairs fertility, due to the local inflammatory conditions that it causes.
Congenital Uterine Abnormalities are a diverse group of anatomical anomalies of the uterus that can vary from simple alterations of the shape of the uterine cavity to uterine septa and cornual malformations. They occur during the formation of the uterus at the embryonic stage of development and are frequently completely asymptomatic. However, they greatly affect the normal anatomy of the uterine cavity, frequently reducing the available endometrial surface and affecting its function.
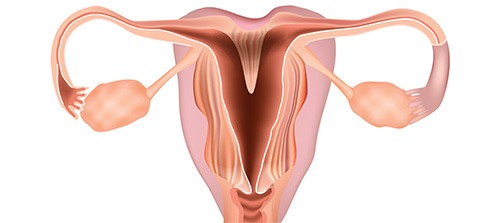
Thus, they may impair fertility by affecting embryo implantation or by causing a miscarriage later on. Additionally, they may affect embryonic development by restricting the available space for growth and may cause complications during delivery. Hysteroscopic repair is the treatment of choice for congenital uterine abnormalities and facilitates the restoration of the anatomy of the uterine cavity back to normal.
Adhesions are abnormal “connections” between normal organs and tissues that consist of connective tissue. They are caused by an “overreaction” of our body to trauma or inflammation, in the attempt to restore normal structure and function. This results in the overproduction of connective tissue around the lesion, which spreads and sticks all surrounding normal structures together.
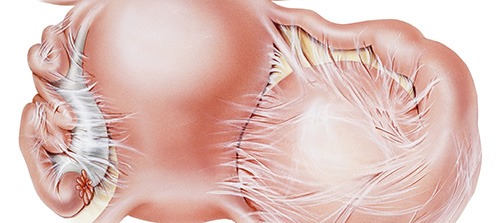
Adhesions in the abdominal and pelvic areas are most frequently caused by previous surgery in the region (particularly if open surgery was performed) or inflammation (a notable example being Chlamydia infection).
Adhesions restrict the movement of the intra-abdominal and pelvic organs and thus may affect functionality. This is particularly relevant in the case of fallopian tube adhesions, which affect tubal peristalsis and thus impair fertilization, while also potentially causing hydrosalpinx and eventually necessitating removal of the whole tube.
EmbryoClinic’s Medical Director, Dr. Elias Tsakos MD, FRCOG and selected members of our Medical Team at EmbryoClinic have been trained and certified in the application of Minimally Invasive Solutions in the treatment of gynaecological conditions that may cause infertility.
Minimally Invasive solutions
Effective, minimally invasive treatment options that combine optimal effectiveness with maximum safety and impeccable aesthetic results.
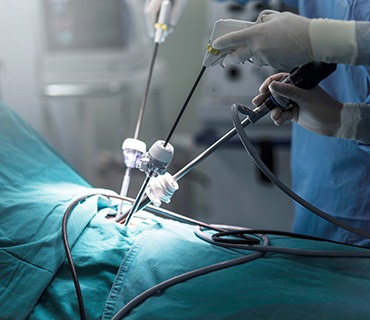
Laparoscopic Surgery
Laparoscopic surgery allows access into the abdominal and pelvic cavity through 4-5 small skin incisions and via an endoscopic camera and surgical instruments enables all necessary surgical manoeuvres. These technical features translate into reduced patient morbidity, compared to conventional open surgery, increased surgical safety and superior aesthetic results with regard to skin incision healing. While laparoscopic surgery aims at treatment, the same methodology may be used for diagnostic purposes as well. Diagnostic laparoscopy is the gold standard in the diagnosis of multiple gynaecological disorders, while simultaneously allowing for direct therapeutic intervention in the same session.
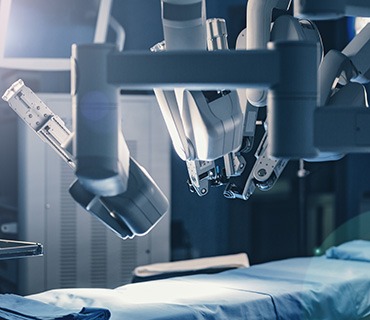
Robotic Surgery
Robotic surgery is the natural evolution of laparoscopic surgery. It offers superior, 3D visualization of the abdominal cavity and precise movements via the control of four robotic arms that bear surgical instruments. This remarkable technology facilitates the performance of complex surgical movements and procedures, which would otherwise necessitate open surgery, while at the same time achieving optimal surgical results with the utmost safety for the patient (reduced complications, blood loss, hospitalisation etc). The minimal burden on healthy tissues, combined with the ability to execute complex surgical manoeuvres is particularly applicable to removal of uterine fibroids and restoration of uterine anatomy in the context of fertility.
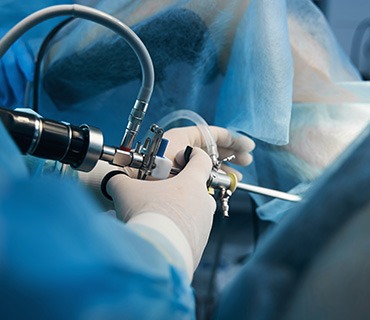
Hysteroscopy
Hysteroscopy, like laparoscopy, may be applied in the context of both diagnosis (see “Female Fertility Assessment”) and treatment, as diagnostic and operative hysteroscopy respectively. Operative hysteroscopy allows for incisionless, minimally invasive intervention via the insertion of an endoscopic camera through the vagina and cervix and into the uterine cavity. It is the only minimally invasive technique that allows for the assessment of the endometrium, the internal lining of the uterus which is of the utmost importance in the context of fertility. Operative hysteroscopy is the method of choice for removing small myomas located right underneath the endometrium and for the treatment of congenital uterine abnormalities.
The GynSurgery Team
Meet GynSurgery, a team of well-trained and highly experienced Gynaecological Surgeons, founded and led by Dr. Elias Tsakos. GynSurgery specializes in fertility surgery and particularly in Minimally Invasive Solutions with a special interest in Robotic Surgery, in addition to general Gynaecological Surgery.
Find out more in our leaflet:
EmbryoClinic is by your side
on every step of your journey
towards parenthood!